Areas of expertise
At the Centre for Health Crises, we work across several areas of expertise in order to address health crises from an ‘all hazards’ perspective and to have a simultaneously short- and long-term focus in our work. To us, health crises arise both from harmful disruptions that occur or are at risk of occurring, and from the vulnerability of health systems. Across all our areas of expertise, we value our strong basis in practical health crisis work.
Definition of a health crisis
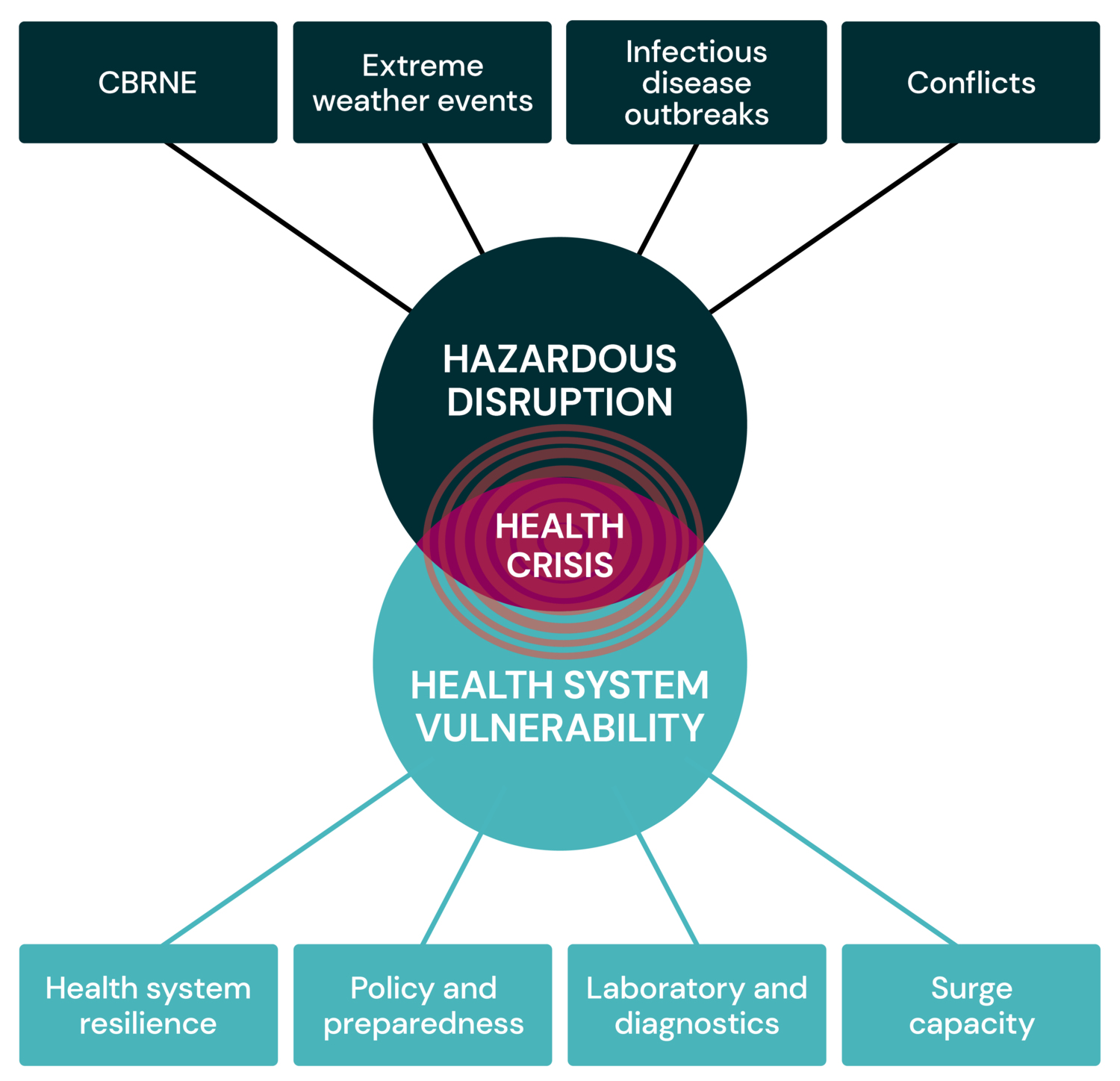
At the Centre for Health Crises, we define a health crisis as:
A hazardous disruption that causes significant effects on human health and that risks exceeding the health system’s ability to cope.
The development of a health crisis, as well as the scale and severity of it, is determined by the disruption, the vulnerability of the affected individuals and health system, and the proportion of exposure in a given context.
We approach health crises from a broad, interdisciplinary perspective and look at health crises in terms of both threats/disruptions and health system vulnerabilities. This allows us to identify and connect trends, solutions and approaches that are relevant to all health crises, which helps to promote better resource utilisation and contributes to a holistic approach to health crisis preparedness and management.
Moreover, our competency is closely linked to practical work in health emergencies and crises. By maintaining a strong connection to operational work in all our areas of expertise and by seconding staff to health emergencies, we continuously expand build our collective expertise.
Areas of expertise
The Centre's competency is built around a number of areas of expertise, in both health system vulnerabilities and health threats/disruptions. Each area is led by an expert coordinator, who has extensive knowledge and networks in their field. All expert coordinators work part-time at the Centre. The rest of the time they work with research, teaching, clinical and practical work in their area of expertise.
The different areas of expertise often collaborate, to benefit from each other's knowledge, create interdisciplinary collaborations and thereby address health crisis issues based on a common approach.
What follows is a presentation of each of our areas of expertise, as well as contact details for each expert coordinator. On the page Work and activities you can read more about our activities and the focus areas we are currently working within. Information and invitations to seminars, workshops and other activities can be found on the home page.

Chemical and toxicological events
Health risks and crises arising from chemical and toxicological events are a serious threat to individuals health and to the environment. Such events include releases of toxic materials, whether in gaseous, liquid, or solid form, resulting from, for example, road accidents, or deliberate releases of toxic materials with the intention of harming people and society. Chemical incidents can create major health crises affecting both individuals and society as a whole.
Preventing such events and managing them appropriately if they occur is crucial for our health and well-being. In this area, we place a strong emphasis on training and partnerships within education, as well as the identification of knowledge gaps.
The work in this area is led by our expert coordinator Mattias Öberg.
Riskzonen
Within this area of expertise, we have produced the fourth season of the podcast Riskzonen. It is a podcast about the dangers that threaten and how we deal with the unpredictability of life.
In the fourth season, each episode focused on a topic related to health crises, such as heat waves, infectious disease outbreaks, or health system resilience. In addition to Mattias, several other members of our team featured on the podcast and shared their expertise and provided insights into how to build preparedness and how to manage health crises. You find Riskzonen on all major podcast platforms.
Mattias Öberg
Expert coordinator chemical and toxicological incidents
Critical care with limited resources
In almost all health crises, regardless of how and why they occur, the need for critical care of patients increases. At the same time, the resources and capacity to provide It often decrease, due to vulnerabilities such as system overload, lack of infrastructure and other uncertainties. Therefore, there is a need to improve and strengthen the ability to provide critical care with limited resources.
A critical care system that is well-prepared, that can scale up and adapt its practices is the basis for adequate health crisis management. We want to promote this through our policy work, contributing to public debate on the topic, participation in expert groups and more.
Work in this area is led by our expert coordinator Märit Halmin.
Märit Halmin
Expert coordinator critical care with limited resources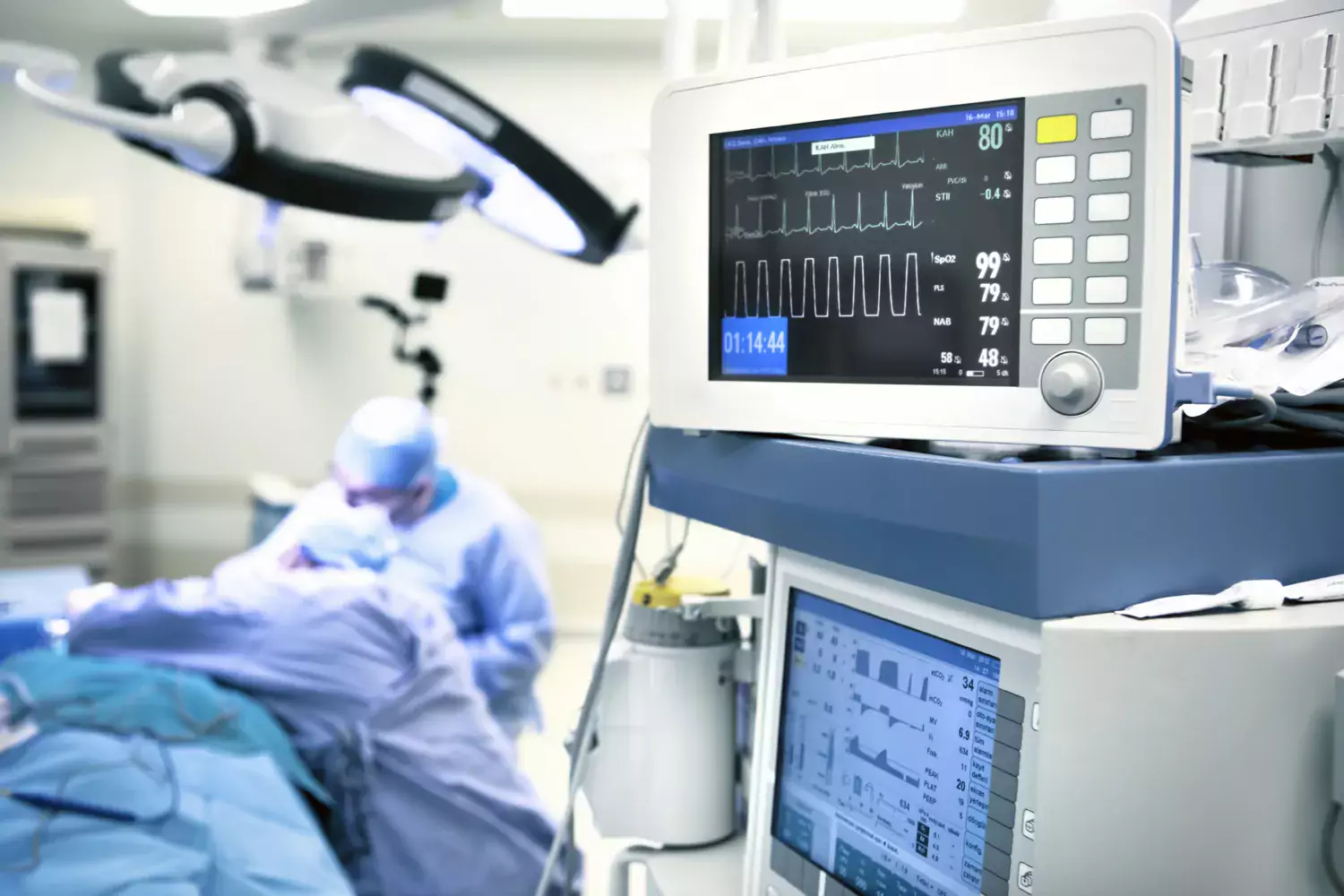
Emergency surgery
Emergency surgery is a frequent feature of many different types of health crises. It requires skills in prioritisation, especially when the needs exceed the available resources, which is often the case in crises and disasters. In our current societal climate, with poly-crises and a move to improve the Swedish total defence capability, the need for the competence and skills of emergency and trauma surgery will increase. Therefore, we want to highlight the importance of maintaining and developing this competence, through education, research, training, and collaboration.
Work in this area is led by our expert coordinator Lisa Strömmer.
Lisa Strömmer
Expert coordinator emergency surgery
Extreme weather, climate, and health effects
Climate change and more frequent extreme weather events, in the form of heat waves, droughts, cold, etc., create significant negative health impacts and are a threat to existing medical infrastructure and practice. Mitigation and adaptation measures need to be implemented and evaluated through multidisciplinary research collaborations, to determine and monitor their effectiveness. In addition, given the already existing magnitude of extreme weather events, we need to understand their impact on human health and how best to prepare for and prevent adverse health effects.
In this area of expertise, we are part of a collaboration on climate and health within the Stockholm Trio university alliance, together with KTH Climate Action Centre, the Bolin Centre at Stockholm University and the Centre for Excellence of Sustainable Health at KI. Furthermore, we work also on catalysing research collaborations within the field.
The work in this area is led by our expert coordinator Petter Ljungman.
Petter Ljungman
Expert coordinator extreme weather, climate and health effects
Health system resilience
A health crisis is determined by the combination of the health threat or hazardous disruption and the vulnerability of the health system. The vulnerability, both of the individual and the community, will determine the ability to prepare, manage and learn from a crisis. How resilient a health system is under normal circumstances affects how and how well it can cope with the unusual and more difficult circumstances that a health crisis creates. Effective and applicable methods to strengthen health systems and improve their resilience will therefore lead to improved preparedness and ability to manage health crises. However, it is important that this is done with an understanding of the context and capabilities of the health system in question.
We work to highlight the importance of health system resilience, both in Sweden and internationally, through training, knowledge dissemination, research and more.
The work in this area is led by our expert coordinator Helena Nordenstedt.
Helena Nordenstedt
Expert coordinator health system resilience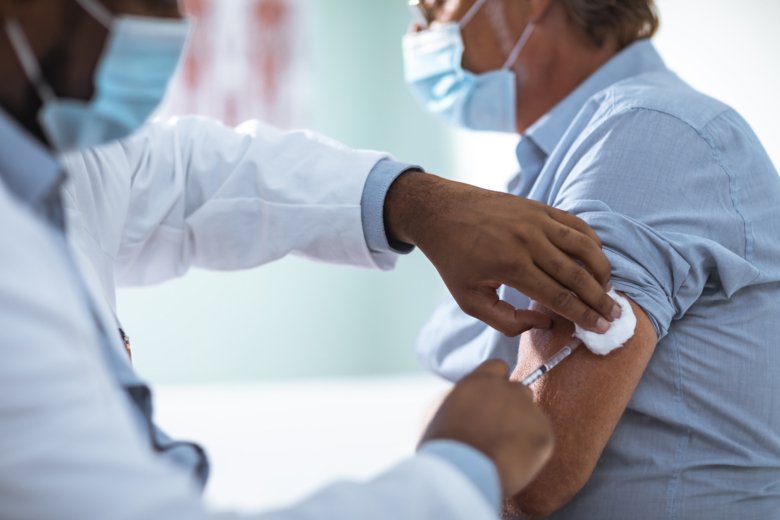
Infectious diseases and vaccine preparedness
Infectious and communicable diseases pose a serious health threat and lead to both local and global health crises, especially if basic health resources and infrastructure are limited. Vaccines are effective and reliable tools to fight many infectious diseases. As such they are an important element of health crisis preparedness, while effective case management and vaccine implementation are equally important once the crisis has occurred.
At the Centre for Health Crises, we want to support initiatives that explore how vaccine competence and vaccine development, vaccine confidence, collaboration, logistics and management can be improved in normal circumstances, and how that then translates into improved capacity to manage a health crisis.
The work in this area is led by our expert coordinator Helena Hervius Askling.
Helena Hervius Askling
Expert coordinator infection and vaccine preparedness
Laboratory and diagnostic surge capacity
The need for laboratory infrastructure and diagnostic capacity is a constant hallmark in many health crises, ranging from infectious diseases to exposure to chemical spills. Additionally, the need to adapt and expand laboratory and diagnostic capacity in times of crisis is another perpetual feature and must be adequately considered to improve our preparedness.
Based on experiences from the COVID-19 pandemic, we want to work to cement and improve surge capacity capabilities in laboratory and diagnostic work, in order to be better prepared when the next health crisis strikes, whatever the source of It may be.
The work in this area is led by our expert coordinator Jessica Alm.
Jessica Alm
Expert coordinator laboratory and diagnostic surge capacity
Outbreak preparedness and response
When a health crisis occurs due to an outbreak of an infectious disease rapid and effective management is crucial. That Is the case regardless of scale of the outbreak. Outbreaks of infectious diseases can be difficult, even impossible, to cure, and far from every outbreak can be prevented with vaccines. Instead, outbreaks can only be managed in the best way possible, in order to prevent an escalating health crisis.
Based on our holistic view of health crises and the importance of health system resilience, the Centre wants to support the strengthen capacities in both preparedness and management of outbreaks of infectious diseases, through, among other things, education, and policy work in the field.
The work in this area is led by our expert coordinator Hedvig Glans.
Hedvig Glans
Expert coordinator outbreak preparedness and response
Policy and preparedness
A health crisis does not occur in a vacuum, but rather within a context. The context will determine the level of preparedness, as well as how the crisis can be managed and how both individuals and society can evaluate and move forward from it. Consequently, it is extremely important to understand how politics, society, and social structures affect preparedness and health crisis management, and what limitations and tools can be used and developed.
At the Centre we want to be a constructive partner in contemporary crisis management and work to stimulate policy development and collaborations, as well as working to set agendas for increased health crisis preparedness. We also want to contribute to creating forums for discussion and learning, through, for example, our policy labs.
The work in this area is led by our expert coordinator Maja Fjaestad.
