Our mission
Karolinska Schizophrenia project is committed to clarifying the roots of the disease and to accelerate the transition from basic biological insights into new therapeutic approaches that impact the daily life of the individuals that suffer from the schizophrenia.
Large-scale unbiased genetic association studies have revealed a growing number of variations in the DNA sequence that associates with schizophrenia. This data offers an unpreceded opportunity to understand disease mechanisms and advance therapeutics. Yet, successful exploitation of these results requires a commitment to invest in disease models that capture the daunting polygenicity of schizophrenia while offering linkage with high-resolution phenotyping.
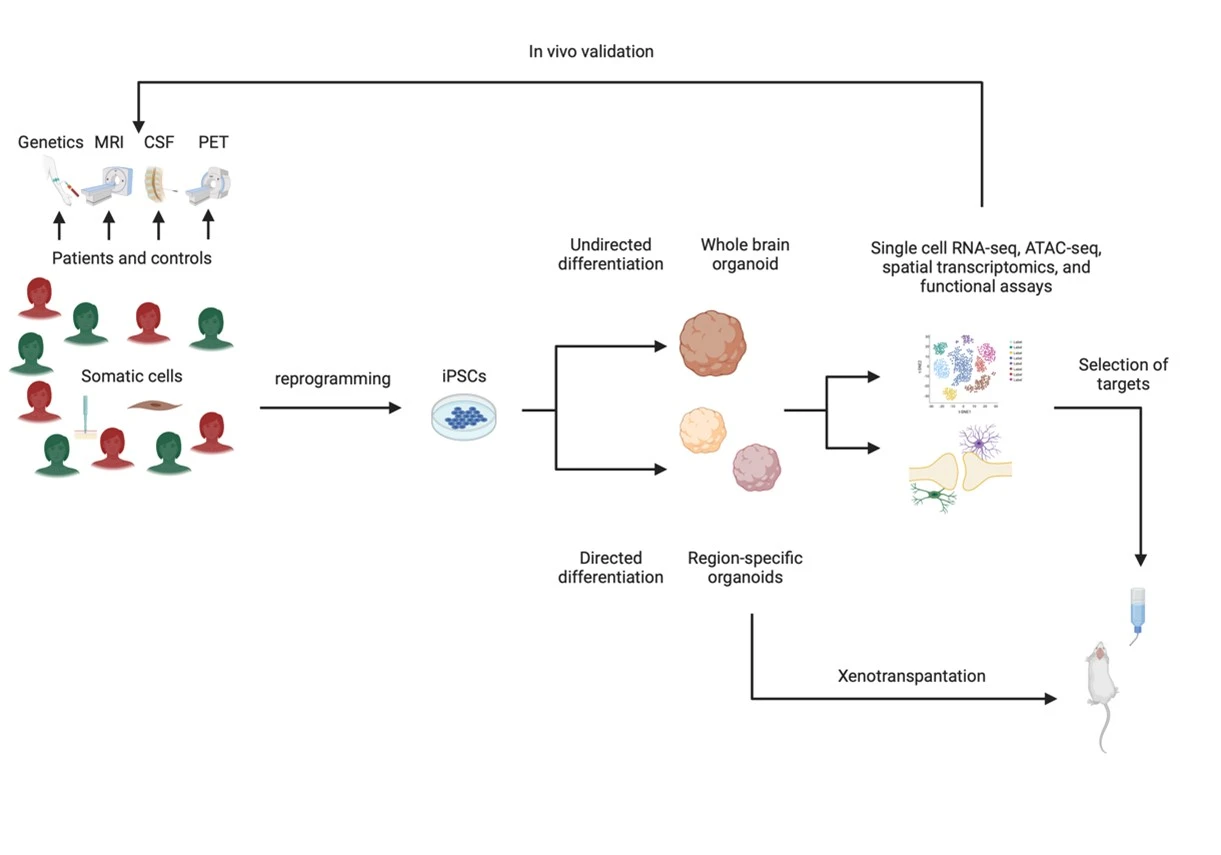
In KaSP, we address these challenges by collecting a variety of biological data from meticulously phenotyped first-episode psychosis and distinguish clinical trajectories by performing follow-up investigations. Experimental models are based on cells obtained from the patients, and by cellular reprogramming we generate models of the developing brain that are unique for each patient. This enables us to translate our experimental findings directly back to each patient by performing e.g., targeted measurements in collected cerebrospinal fluid our by analyzing collected brain imaging (MRI and PET) data and ensure relevance for the living human brain. To cover aspects that are lost in the dish, our in vitro models are also complemented by animal models, in which we also transplant patient-derived brain organoids.
