Curious about viruses
Some viruses make us sick, others are harmless stowaways, and some play an important part in our ecosystems. They can also be used for medical purposes and possibly as a weapon against multi-resistant bacteria. Impressive for something so small that it is not even really alive!
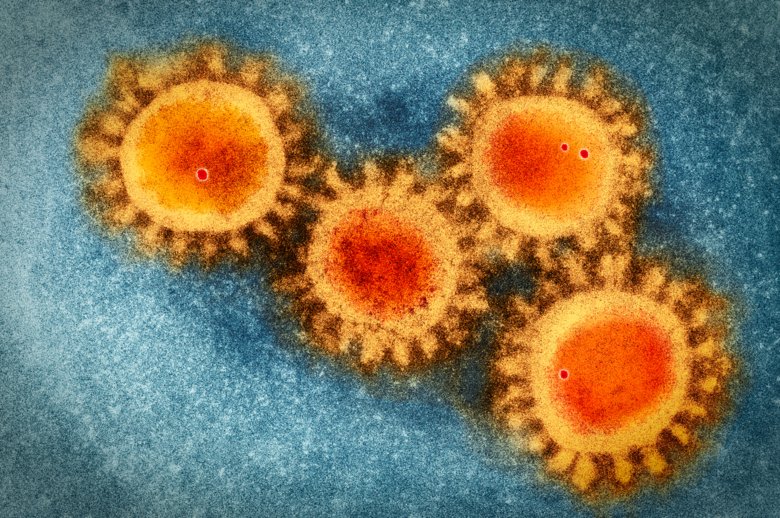
Viruses are the world´s smallest and probably most common life form, if we allow ourselves a generous interpretation of the term “life form”. Viruses might not fully fit our definition of life, but at the same time, it is too reminiscent of life to be described as dead matter. They are something in-between. A snippet of genetic code, without a cell and metabolism of their own, but with an ability to reproduce, develop and spread across the world.
Viruses are around 100 to 1,000 times smaller than bacteria and remained undiscovered until the 1930s. That was when the electron microscope was invented, which is significantly more powerful than a light microscope.

“Before that, you did not know if there was anything there, a sort of infection that remained after all bacteria had been filtered away, but there was no knowledge of what it consisted of,” says Anna Smed Sörensen, associate professor in immunology at the Department of Medicine, Solna, Karolinska Institutet.
She is researching how our immune system reacts to phenomena such as viruses.
“It is often the response from the immune system that causes us to feel ill during an infection,” she says. But things would be even worse if the virus was not fended off, as there are many dangerous consequences of an infected organ losing functionality.
Successful virus treatments have existed for far longer than knowledge of viruses. The first vaccine, used to fight the viral disease smallpox, began seeing use more than 200 years ago, after doctor Edward Jenner had shown that people who were exposed to cowpox became immune to smallpox. Before that, vaccine-like methods, variolisation, had been used for similar purposes for hundreds of years in countries such as China or India.
Almost two centuries after Jenner’s experiments, smallpox became the first disease that man was able to exterminate. Victory was publicly declared by the World Health Organisation (WHO) in 1980. The last outbreak of smallpox in Sweden took place in 1963.
Most are not dangerous
Viruses are often linked with disease, but that is somewhat unfair, says Anna Smed Sörensen.
“There are many, many viruses in the world. But only a tiny amount of them infect humans, and only a small fraction of these make us sick. But naturally, these are the ones that have been most thoroughly researched, and to some extent viruses that affect important pets and crops. We do not know all that much about the other viruses in the world.”
All forms of life on earth – animals, plants, mushrooms and bacteria – have their own virus types, and most things point to virus particles being the most numerous by far.
Viruses play an important role in the ocean ecosystems, where they infect and blow up phytoplankton at dizzying speeds. But there is still plenty to discover about viruses’ role in ecosystems. This also applies to the ecosystem of the human body, according to Anna Smed Sörensen.
“The good bacterial flora has become a hot research field, but we still do not know the benefits of our viral flora. You could for example imagine a virus that infects bacteria being important in the regulation of our bacterial flora. Other research groups are working on such issues, and I believe that we will know much more within just a few years. There is a lot happening now regarding virus research in general, because we have gotten really great tools over the last few decades,” she says.
Some viruses have followed humanity throughout history. Others, such as the new coronavirus, SARS-COV-2, have just made the leap to our species. How the virus acts within our body can reveal something about the duration of our shared history, Anna Smed Sörensen explains.
“Viruses that have been around for a long time are generally more sophisticated,” she says. They can be better at not agitating the immune system and remain in the body as a chronic infection. New viruses have not had time to develop the same level of finesse, instead they cause a severe immune response and acute illness. This is a worse strategy for the virus.
The viruses that are now stowaways in our genes are the ones that have developed the most.
“A fairly large part of the human DNA is actually old retroviruses that have managed to copy themselves into our genome,” says Anna Smed Sörensen. They are generally no longer active and normally does not affect us.
Two weapons against viruses
In the fight against viral diseases, medical science has two weapons at their disposal: vaccines and antivirals. Following Jenner’s smallpox vaccine, a number of vaccines against other serious diseases have followed. One example is the polio vaccine, which has eradicated the disease in most parts of the world since its introduction in the 1950s. There are hopes that the polio virus will be the third virus to be exterminated, with the first two being smallpox and the animal disease rinderpest. The last major outbreak of polio in Sweden was in 1953–1954, where more than 3,000 people suffered paralysis. According to WHO’s calculations, vaccines prevent between two and three million deaths every year.
The second weapon for combating viruses, antivirals, are aimed at fighting ongoing infections. Some of them are curative, others have anti-retroviral effects that do not remove the virus completely, but keeps the infection in check. Antivirals have a significantly shorter history than vaccines. Anders Sönnerborg, now a professor in infectious medicine and clinical virology at the Department of Medicine, Huddinge, Karolinska Institutet, was a freshly baked physician when the first antivirals started being used in healthcare in the early 1980s.
“The first really effective antiviral drug was the herpes medicine called Aciclovir,” he says. It was very successful and is still being used today. It is not a curative drug, but highly effective against the symptoms.
The success of Aciclovir lead to high expectations of the research into antivirals.
“There was a period when there were hopes of all viral infections being treatable in the future,” Anders Sönnerborg reminisces. Major investments were made into drugs against cold viruses. The results never came however, and many actors eventually discontinued their virus research.
But towards the end of the 1980s and early 1990s, two events coincided: a new deadly infection, HIV, spread across the world at an alarming rate, while technological developments in molecular biology and IT began to take off.
“HIV research grew quickly and utilised the opportunities that the new technology provided,” says Anders Sönnerborg. In many respects, it became the starting point for modern virus research. For example, it was the first time computer-based simulations were used to figure out what a drug should look like, instead of blindly using trial and error. It was revolutionary.
Today, there are antivirals against many viruses, including herpes, HIV, hepatitis B, hepatitis C and influenza and RS viruses, as well as a number of viruses less known to the public. Anders Sönnerborg is the chairman of a Swedish group of experts that outline recommendations for how the drugs should be used.

“We have a solid and well-used arsenal of antivirals for chronic illnesses,” he says. Use for acute infections is limited, mainly due to the time aspect. The drug treatment needs to start early to have a major impact. This is why use of antivirals against influenza is fairly rare, despite existing.
But for some patients, they are vital, as he points out.
“Viruses that most people can handle can be life-threatening for people with compromised immune-systems, such as people who have had radiotherapy or received a transplanted organ. For them, antivirals against diseases such as influenza and other less common viruses can be life-saving.
Antivirals blocks a step in the virus’s chain of reproducing and infecting new cells. Unlike vaccines, which are normally very specific, they have the potential to strike against a wide array of viruses.
“There are certain mechanisms in a virus that cannot change, which makes them shared among a whole group”, Anders Sönnerborg explains.
Mutations taking place there are always worse for the virus, which is why there is no variation. This is a weakness that can be exploited. Antivirals that blocks this kind of mechanism strike against this whole group of viruses. Today, an important area of research is to develop these so called broad spectrum antivirals.
Changed animal viruses can infect humans
Virus researcher Ali Mirazimi is splitting his duties between the Public Health Agency, the National Veterinary Institute and Karolinska Institutet, here he is an adjunct professor in virology at the Department of Laboratory Medicine. He is involved in research of tests, antivirals and SARS-COV-2 vaccines.
Chinese animal markets being pointed out at the most likely source of the virus is no coincidence, he explains. When humans are afflicted with a new virus, its is most likely an animal virus that has changed, and the most beneficial environment for such changes is where humans and many animal species are crammed together in a small space.

“Different species get each other’s viruses and a diversity of mutations leads to them occasionally being able to survive in a new host. Viruses that encounter each other can exchange genetic material. Large, cramped markets for living, wild animals are therefore the perfect breeding ground for new infections.
But what about the bats? How come that bats have been mentioned as a suspected source of viruses, from Ebola to COVID-19? Do they carry an extra large amount of viruses?
Well, more so than anything, they are very common. The 1,200 species of bat found throughout the world make up one fifth of all mammal species. They are only outnumbered by the rodents, and they also spread many viruses.
Some viruses are very selective and only infect one species, others can live in many different species. They often only cause disease is some of them.
“One of the viruses I am researching, the Crimean-Congo haemorrhagic fever, thrives in everything from ticks and some birds to mammals and humans. But what we do know is that only one species gets sick: humans,” says Ali Mirazimi.
However, there are limits. Viruses for plants and bacteria can, as far as we know, never infect humans. Our cells are far too different. Body temperature is also important, which is why it is not likely that a warm-blooded animal like a human will be infected by a fish virus, for example.
Coughs spreads viruses effectively
Once a virus has made the leap from animal to human – what then determines whether the infection will spread to a limited population or cause a full blown pandemic?
“The main factor is how the infection is spread,” says Ali Mirazimi. The new coronavirus being spread through coughs and sneezing is no coincidence, it is the ideal way. This means that people are spreading the virus at all times through the air around them, which makes it very difficult to avoid infection, something we have seen over the course of the spring. The second best option for the virus is oral-faecal infection, such as the winter vomiting bug.
He points out that another important part is how sick the infected become.
“The SARS virus of 2003 was very aggressive. More or less everyone who become infected ended up in a hospital. This meant that the virus could never really get a foothold among the population. The milder the symptoms, the easier it is for a virus to spread.”
The final determining factor is geography.
“In rural Gabon or Siberia, there are excellent conditions for limiting an outbreak to individual villages. But an infection in Hong Kong makes things more difficult. Then it can appear anywhere in the world the next day.
Viruses do not actually seek to makes things difficult for us, Ali Mirazimi stresses.
“The best thing for a virus is that its host is alive and doing well,” he says. Some cause symptoms in order to spread, but other than that, they do not really want to screw with us. When a virus kills, it does so by mistake, so to speak. This is often because it has been removed from its natural environment. The Ebola virus peacefully coexists with the bats in which it normally resides, but becomes deadly when it happens to en up in apes or humans.
Another reason to look more forgivingly at viruses is that they can be of use to us. Viruses’ ability to introduce new DNA to cells have already made them useful tools in genetic engineering. There has been a lot of talk of bacterial viruses, so called bacteriophages, as a possible weapon against dangerous bacteria. Bacteriophages have proven difficult to tame, but under better technological conditions and a growing number of issues with antibiotic resistance, interest in the field of research is growing.
Three theories on the origin of viruses
Where do viruses come from? How were they created to begin with? We do not know, but there have been (at least) three proposed theories. It is possible for several of these theories to be true. Viruses can have arisen multiple times, in different ways.
- Viruses can be genomes on the run. A small part of a cell which happens to have gained the ability to travel between cells, which led to it forging its own path through evolution.
- Viruses can be a former living organism that went on an extreme diet. Other microorganisms, such as the chlamydia bacterium, have done the same thing but not quite as radically. They have rationalised away parts of themselves to instead live as parasites inside the cells of other species. The mitochondria, the powerhouses of our cells, are also believed to once have been their own organisms.
- The viruses might have been there first! Today, many researchers believe that the first life forms on hearth were not DNA-based, but RNA-based – similar to many viruses. Viruses being something in-between life and non-life could be because they originate from this very first phase of life’s development. A proto-life that never continued evolving towards life, but still became successful.
Source: Wessner, D. R. (2010) The Origins of Viruses. Nature Education 3(9):37
Text: Anders Nilsson. First published in Medicinsk Vetenskap nr 2 2020
Related reading
 Photo: Getty images
Photo: Getty imagesThe evolution of virus variants
Hopefully we are nearing the end of the pandemic. But the virus is still there and scientists expect that new variants may emerge. Making us more sick, however, is not on the viral agenda.
 Photo: Ulf Sirborn
Photo: Ulf SirbornWhy we react differently to COVID-19
One of the striking features of COVID-19 is the big differences between how we react to being infected with SARS-CoV-2. Some show no symptoms, while others get seriously ill and die. The international career-network Academic Positions interviewed KI researcher Anna Smed-Sörensen to find out more about more.
